Microneedling’s popularity shows no sign of slowing. Amanda Pauley explores the science and safety precautions to be aware of
Amanda Pauley
microneedling
Microneedling, also referred to as Collagen Induction Therapy (CIT) or medical skin needling, is a sought-after treatment, with celebrities such as Gwyneth Paltrow and Naomi Watts swearing by its anti-ageing benefits. But why has it become so popular with both clients and salons?
“Clients are seeing it as a great alternative to more abrasive treatments such as laser and chemical peels, and it’s more cost-effective for salon and clinic owners – it’s a treatment they can achieve great results with but with minimal outlay,” says Emma Bennett, owner of Advanced Facialist, based at the Amida Spa in London’s Chelsea Harbour Club, and founder of The Therapist Finishing School in Fulham.
The procedure, which can take anywhere between 30 and 60 minutes, claims to fight the signs of ageing and reduce skin laxity by stimulating the body’s own collagen production. “Using precision needles, the therapist makes thousands of micro-channels in the skin, which causes the body to think it’s being attacked,” says Sharon McCormack, lead trainer for Nouveau Skin Therapy, which distributes microneedling device Dermatude Meta Therapy.
“It then sends new fibroblast cells, collagen and elastin to the surface of the skin, which plumps out fine lines and wrinkles as well as decreasing any scarring. Also, because the body heals itself and there are no chemicals involved, you can promote it as a natural treatment even though it’s slightly invasive,” she adds.
Needle lengths start from 0.25mm and therapists can use anything up to a 1mm, with 1.5mm and above generally classed as medical. “We suggest no higher than 1mm on the face and 1.5mm on the body,” says Sharon Hilditch, managing director of machines manufacturer Crystal Clear. “However, medical practitioners or Level 4-trained practitioners can use more than 1mm on the face.”
Bennett says that therapists commonly use 0.5mm and “they’re taught in training that they shouldn’t use more than 1mm, but there’s not actually any laws stopping people. It’s a grey area.”
Who is it best for?
Although primarily used on the face, the treatment can be conducted anywhere on the body and is suitable for all skin types and colours. It can treat a variety of skinconditions, from deep wrinkles to sun damage and pigmentation, and is particularly effective on scars.
“You can be much more tailored with scars, but you need to treat them at a depth of between 0.5mm and 1mm to make a difference. However, each scar will be a different depth, so using a different needle length on each is ideal to get the best results,” says Bennett. “For example, clients tend to get deeper scars on their cheeks because there’s more flesh, while those on the forehead are less deep.”
The treatment’s biggest appeal has to be that it’s well tolerated and comes with minimal downtime – normally around 24 to 48 hours. “As a practitioner, you can guarantee all the benefits of skin rejuvenation while minimising the risk of dehydration, decreased cell functioning, infection and other side effects associated with many other wounding treatments,” explains Kathy Taylor-Brewin, managing director of BioActive Aesthetics, which distributes microneedling device SkinPen Precision.
Are there any contraindications?
Despite the treatment’s inclusive feel, there are some contraindications to watch out for – from pregnancy, heart disease and open wounds, to cold sores and active acne. “Clients who have quite bad scarring from acne find that microneedling helps resurface the skin, but I would never skin needle on someone with active acne as the pustules are full of bacteria and you don’t want to spread that around,” says McCormack.
However, if the acne isn’t active, you should make clients aware that microneedling could bring on an onset. “The negative of doing the treatment on someone with acne is that you have to warn them that it could get worse before it gets better, but from a clinical view that’s exactly what you want,” explains Andrew Hansford, aesthetic practitioner and founder of ACH Aesthetics training academy and clinic. “The oil and sebum is being pushed up from the epidermis to the top layers of skin but then evens out so that the acne is pretty much gone and you can treat the scars.”
The same precautions should be taken with clients who suffer from cold sores. “I would do the treatment at around four to six weeks after a cold sore episode,” explains Bennett. “But, if the client is regularly prone to them, I would make them aware that it’s a possibility that microneedling could stimulate the condition.”
Which device should I use?
There are three main types of tools you can use for the treatment, the most well-known being the dermal roller. The roller is an operator-dependent, disposable tool that a therapist rolls over the client’s skin to produce thousands of microscopic needle holes diagonally in the dermis, generating new cells.
“Dermal rollers are the best starting point cost-wise for therapists to set up and have training, and for most clinics, I think it’s their entry point,” says Bennett. However, the experts agree that with this device quality training is vital. “If you press too hard you can cause those derma channels to go too deep in the wrong places and could end up with excess bleeding or scarring, but if taught properly, therapists can get really good results,” explains McCormack.
Another favoured tool is the needling pen – a mechanical device which comprises multiple needles that vertically pierce the skin – and most feature a guide for therapists to set the depth they need. “You set the needle length on the guide, for example 0.5mm, and that is as deep as the needles would go,” says McCormack. The pens also have a guard that “contracts the needles back into the pen once the therapist has stopped the treatment, so the risk of needlestick injury is near impossible. You would have to shove your finger into it to get caught,” explains Hansford.
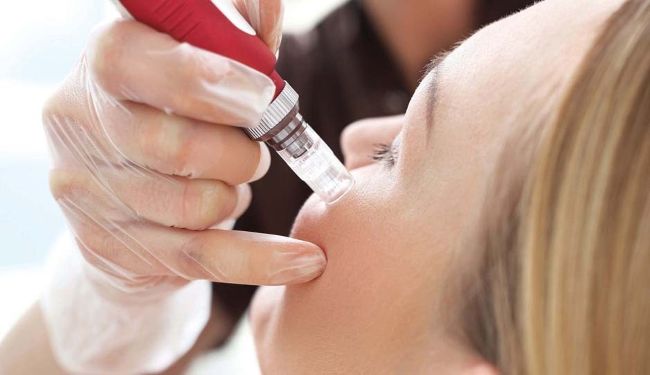

Many salon owners are also opting for this device as it allows them to target the point of entry more precisely. “The needles are going in and out a lot quicker so you can move on from an area much faster while causing the same number of channels as with other devices,” says McCormack, while “the flexibility of changing the needle length on different parts of the face when required means the therapist can target areas such as the skin around the eyes and forehead better,” says Taylor- Brewin. However, “the pens tend to be more expensive to invest in than the rollers,” says Bennett.
Lastly, there is the derma stamp – a tool which works by stamping the skin with microneedles to cause the natural wound healing process. “It stamps the skin, straight in and out, with a vertical application. It gives a good result but not many people use this device anymore,” says Hansford. “Also, because it’s a block, you can’t really get around the eye area or the creases of the nose, so you’re limited to where you can work.”
What infection control should I be doing?
In January, Government agency Public Health England (PHE) announced it was investigating the possible risk of blood-borne viruses being transmitted during skin needling after three staff members in beauty salons in the North West reported needlestick injuries from disassembling a device that combines dermal rollering with the infusion of ingredients.
Although this has put safety in all types of needling treatments in the spotlight, therapists shouldn’t feel nervous about conducting the procedure. “There is very little to worry about,” says Hansford. “The treatment is very safe when done in the right hands.” Hilditch agrees and thinks a firmer focus on best practice and high standards is the way forward. “The safety of both client and practitioner is paramount with any microneedling procedure and a strict protocol needs to be followed to ensure total hygiene.”
In every treatment, therapists should tie their hair back, use good lighting, wear protective gear – apron and face mask – and “change their gloves regularly so they’ve got less chance of contaminating themselves or anyone else”, says McCormack. As an added safety measure, you could wear nitrile gloves because they’re thicker, but “if practitioners are taught best practice in their training then there should be no issues. They should never need to touch the needle points,” says Hilditch.
The treatment environment should be clean and the device being used in a sterile packet. “I always show my clients that the tool is fresh from the pack so they know I’m handling the situation with the utmost care,” adds Bennett. Everything used in treatment should be onetime use only – from needles to wipes – and the tools should be disposed of in a sharps bin, not general waste. “Disposing of everything correctly is crucial,” adds Bennett. “You need to contact your local council to arrange for a collection for your sharps bin and that should be done on a weekly basis.”
What should I do if I get a needlestick injury?
The experts say the protocol is to stop the treatment, remove your gloves and place a clean, sterile glove on the hand that’s not injured before assessing the skin on the other to see if it’s broken. “If you have broken the skin then you need to flush it out. Squeeze it under a running tap for a few minutes, before drying it and placing any materials you’ve used, or that have particles on, into a hazardous waste bin,” explains McCormack. “You then need to put a plaster on the cut, cover with a sterile glove and then clear the work station.”
You also need to make the client aware of what’s happened. “Apologise and explain the situation, then double check to see if they’ve missed anything off the medical health form,” adds Hansford. As well as putting the incident into your accident record book, you also need to advise the client to go to A&E or visit their doctor to be checked out. “But, you also need to get yourself checked,” adds Bennett. “Once you and the client have been given the all clear, you can book them back in again for the treatment once everything has healed.”